For decades, scientists have known that the pancreas undergoes microscopic changes as type 2 diabetes develops—but most of those changes are so subtle that classic histopathological exams can’t reliably detect them. What if we had a tool that could zoom in on these faint morphological signals and make sense of them at scale? A team from the German Center for Diabetes Research (Deutsches Zentrum für Diabetesforschung; DZD) and collaborators has now built exactly that. Their new AI‑based approach reveals previously hidden tissue features associated with impaired insulin secretion and beta‑cell dysfunction, offering a fresh window into the early biology of type 2 diabetes.
The study, published in Nature Communications and titled “Explainable AI-based analysis of human pancreas sections identifies traits of type 2 diabetes,” tackles a long‑standing diagnostic challenge. Classic histopathology—the visual inspection of stained tissue under a microscope—has never been particularly effective at distinguishing pancreatic tissue from people with and without type 2 diabetes. Complicating matters further, accessing human pancreatic tissue from living donors is notoriously difficult: the pancreas sits deep in the abdomen, and biopsies or resections carry significant risks. As a result, most research has relied on post‑mortem samples, which can obscure the very early changes scientists hope to understand.
To overcome this limitation, the researchers assembled one of the most extensive human pancreatic tissue datasets to date. All samples came from living donors, an important detail because it avoids the distortions that can occur in post‑mortem tissue. Each section was processed using both chromogenic staining and multiplex immunofluorescence, techniques that highlight different cellular structures and molecular markers. The stained slides were then captured using gigapixel microscopy.
With this dataset in hand, the team trained deep learning models to classify tissue samples as diabetic or non‑diabetic. The models performed remarkably well, reliably distinguishing between the two groups. But the real breakthrough came from the use of explainable AI, which allowed the researchers not only to make predictions but also to understand why the model made them.
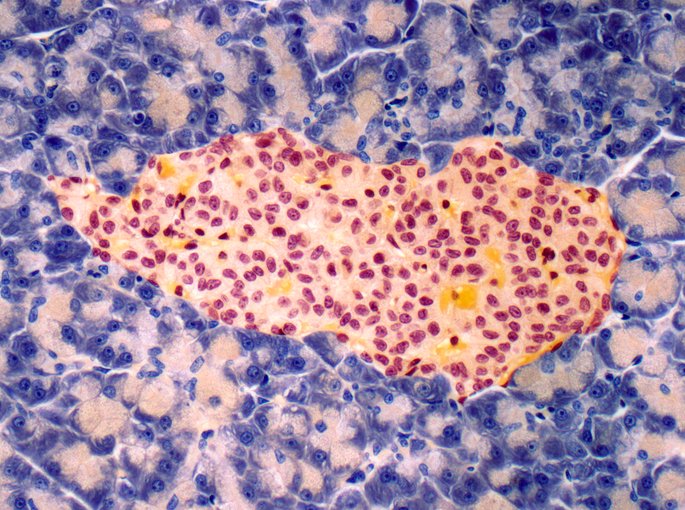
The AI highlighted several tissue features that appear to play a central role in type 2 diabetes. These included alterations in the islets of Langerhans, as well as changes in α‑cells and δ‑cells. “Remarkably, the highest prediction performance is achieved by simultaneously focusing on islet α– and δ-cells and neuronal axons, alongside subtle pancreatic alterations in T2D donors such as larger adipocyte clusters, altered islet-adipocyte proximity and smaller islets,” wrote the authors.
By quantifying these features and describing them as potential biomarkers, the researchers have created a data‑driven foundation for future diagnostic and therapeutic exploration. Their approach doesn’t replace traditional pathology, but it augments it with a level of precision and interpretability that was previously out of reach.
As type 2 diabetes continues to affect approximately 500 million people worldwide, tools that can illuminate its earliest tissue‑level changes are urgently needed. This study shows that AI may be uniquely suited to that task, not just detecting what the human eye can’t see, but explaining what it finds in ways that deepen our understanding of the disease.
The post AI Maps Subtle Human Pancreatic Tissue Changes Linked to Type 2 Diabetes appeared first on GEN – Genetic Engineering and Biotechnology News.